Cholera cases have continued to be recorded in some states in Nigeria. The Nigeria Centre for Disease Control Director-General, Dr. Chikwe Ihekweazu, listed Bauchi, Plateau, Kano, Niger, Zamfara and Kaduna as some of the affected states.
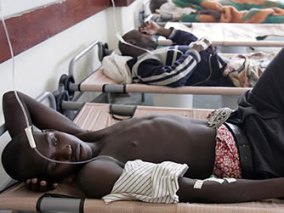
The Federal Capital Territory Minister of State, Dr. Ramatu Aliyu, said 60 persons died of suspected cholera in six area councils, adding that suspected cases had risen to 698. In Plateau State, the disease has killed 21 people and infected 1,144 in two months as of Wednesday.
The World Health Organisation described cholera as an acute diarrhoeal infection caused by ingestion of food or water contaminated with the bacterium vibrio cholerae.
It was gathered that the disease was first reported in Jos North Local Government Area in May 2021.
However, within two months the disease has spread to 13 other local government areas.
With the exception of four council areas such as Mikang, Lantang South, Pankshin and Kanke, other LGAs that have been affected by the disease, as noted by the state Commissioner for Health, Dr. Nimkong Lar, were Jos North, Jos South, Riyom, Kanam, Bokkos, Wase, Mangu, Bassa, Jos East, Barkin Ladi, Qua’anpan, Langtang North and Shendam.
Findings also showed that most of the infections were recorded in rural communities while all the dead victims were said to be those who didn’t report to the hospital on time for treatment.
Some of the doctors treating cholera patients in the state talked about their experiences.
An infectious disease expert at the Jos University Teaching Hospital, Dr. Inanayi Bitrus, described the disease as real in the state.
He said, “Some people don’t take it seriously when they hear that there are cases of cholera in some states including Plateau. It is unfortunate because it is already with us in Plateau.’’
Bitrus stated that when the bacteria entered the human body, it would secrete toxins to cause severe diarrhoea, vomiting and dehydration to the host.
He said, “The type of diarrhoea is different from the normal one. This one is like rice water which is peculiar to cholera disease. The patient is sometimes presented with increased diarrhoea in a day and some lose a lot of water in the body. When such happens, the people need to come to the hospital immediately to avoid extreme cases.’’
Bitrus, who said he had treated about eight cholera patients since the disease started in the state, added,” Usually when patients come to the hospital especially in the accident and emergency ward, they present symptoms such as vomiting and passage of loose stool and most times, the presentation is like rice-water stool. Rice water stool is associated with cholera. At the initial stage, the patient is passing stool, there will be faecal material and as time goes on, when everything has been expelled, one will discover that the patient will become weak.
“So because of the cases, there is a high index of suspicion. What we normally do is to keep the patient in a secluded area within the hospital and run a test and we can get the results within a few minutes. Most times, the major challenge of these patients is fluid because they vomit and pass loose stool. The main thing they need is rehydration.
“I treated eight patients during my call duty. The test kits and antibiotics are available. Most times, the challenges are on the side of the patients who sometimes report to hospitals late and some of them could not afford the fluid. I remember that there was a patient that came highly dehydrated and in shock. Within 24 hours, I was able to give the patient over 20 litres of fluid and that is much. And most of the patients are from the rural communities, peasants who don’t have much to support themselves.”
Also sharing his experience treating patients, the Medical Superintendent, Bokkos Hospital, Dr. Ayuba Tongswan, said not many people had reported for treatment since the disease occurred.
He said, “We have a few cases in the hospital and we are treating them as they come. The situation here is a little bit worrisome and over the week, we had like five cases. When we have such cases, we usually call the LGA disease surveillance officer who records the situation. But I can tell you that nobody has died from the disease in our hospital.’’
On his part, Dr. Nathaniel Dusu of Riyom General Hospital told one of our correspondents that they had been placed on red alert to attend to patients with cholera.
Dusu stated, “We were told to be on standby in case of an emergency since the disease started, but for now, we don’t have any patient on admission for the disease in the hospital though there are other patients.’’
One of our correspondents visited the primary health centres in Vwang District, Jos South Local Government Area of the state.
One of the doctors who spoke on condition of anonymity lamented the increase in cholera patients in the state.
The doctor who said he had handled cholera cases in the past five years said that almost every year, the state battled the disease.
The doctor said, “Most of the patients come from rural communities where there is no potable water. In the villages, they drink water from the stream. Why can’t the government do something about the situation?”
“The first patient I treated during this period was someone I met when we went for medical outreach in the Barkin Ladi community. He was brought by a relative and after treatment; he was okay. He told me that he drank from a stream because it is the only source of water in their area. I think the disease can be tackled if the government makes provision for good drinking water, especially for rural dwellers. The government should help the affected communities.
“The best way to avoid the disease is sanitation. Most times, the mode of transmission is from faeces to the mouth caused by poor sanitary conditions within an environment especially where there is still open dumping of refuse. If the patient gets water from the stream or well and the faeces mix with it especially during the rainy season, using such water could lead to an infection. Another thing is that some people who buy fruits from the market don’t wash them properly before eating.’’
The state Commissioner for Health, Dr. Nimkong Lar, however, blamed the cholera cases on carelessness and rule violation by the people.
He stated, “The people should be careful about whatever they do. We are trying to enlighten the public on how to prevent contracting cholera and what to do when such incidents occur. The people are not following the rules and that’s why the problem has lingered. There is a need for people to cover their food to stop flies from perching on it. Their faeces should be discarded properly.
“You also find out that people with the disease usually don’t report themselves to the hospital to enable them to get treatment early enough. I can tell you that those who had the disease were those who did not come to the hospital for treatment. Those who came to hospitals were treated accordingly and later discharged. It is important for people to know that the disease is not a terminal one and that reporting at a hospital would save their lives.’’
He added that in some days at the peak of the disease, the state was having about 20 to 30 cases per day, noting that it had reduced.
Lar added, “At a point, we invited officials from the NCDC to the state and they did many things to assist us in curtailing the disease. We are working hard to ensure the stoppage of open defecation which is also associated with the disease. The government is doing a lot to address the incident.’’
On his part, the state Chairman of the Nigerian Medical Association, Dr. Innocent Emmanuel, said that the involvement of the association’s members in the fight against cholera was informed by the prevailing situation which required collective efforts to tackle.
He expressed the hope that the state would overcome the challenge, adding that “Our members are involved and we have been interacting with them and from the feedback, we hope the fight against the outbreak will succeed.’’
All hands to the pump in Bauchi
The then Commissioner for Health in Bauchi State, Dr. Aliyu Maigoro, on May 24, 2021, announced the occurrence of cholera in the state.
Addressing a press conference, he said the index case in the state was recorded on April 24, 2021, in the Magami community, in Burra Ward of Ningi Local Government Area, at a health facility. He added that the patient complained of abdominal pain, watery diarrhoea, and vomiting.
Since the index case, there have been cases across the state with the cases rising to 322 with 20 deaths within the first one month recorded in Bauchi, Ningi, Warji and Giade council areas.
As of July 18, the cases had spread to 16 LGAs and the number of deaths rose to 42 with 2,874 infections. Bauchi LGA had the highest case rate of 2,185 and 22 deaths followed by Toro, Tafawa Balewa and Darazo LGAs.
Investigations by Saturday PUNCH showed that most of those affected were children, particularly almajirai who were mostly in the Bauchi metropolis.
It was gathered that the situation was caused by the fact that the almajirai had no access to good hygiene, water, drink and food. Another issue is the lack of pipe-borne water in the Bauchi metropolis caused by the ongoing upgrade and expansion of water from the Gubi Water Treatment Plant by the Bauchi State government.
The delay in rainfall across the state was also seen as a factor that contributed to the spread of the disease. People were left with no choice but to get water for drinking, cooking and other domestic activities from unclean sources.
Another factor responsible is environmental pollution caused by indiscriminate dumping of waste by residents on the streets, highways and water channels. Running water then washes the wastes into uncovered wells, streams and rivers where residents fetch for drinking, washing, cooking and other uses without purification.
An Infectious Disease Specialist, working with the Abubakar Tafawa Balewa University Teaching Hospital, Bauchi, Dr. Ibrahim Maigari, said most of the cases at the hospital were paediatric, mostly of children less than 10 years.
He said: “What we observed is most of them are usually from the almajiri group. Most of them are homeless, they live in crowded settings. Based on the history that we obtained from them, most of their sources of water are not potable, it is not usually clean. They get their water from wells that are not properly protected. When there is rainfall, usually it pushes dirty water into wells and most of the children, where they live, lack proper places to defecate. Usually, they don’t have an appropriate place to defecate.
“When there’s open defecation and you have rainfall, it washes away those things, and the next thing is that if there are uncovered wells, the water can be pushed into them and they get contaminated.’’
Maigari advised residents to be more cautious and promote healthy practices, adding that people need to know what cholera was, how it’s transmitted and how to protect themselves.
He advised, “One major thing for us to protect ourselves is frequent hand washing and cleaning of food items. When you buy fresh food items, you have to wash or clean them well before consuming them. When you want to drink water, you should make sure you decontaminate it. Don’t just drink water without knowing its source.’’
The Director-General, Bauchi State Environmental Protection Agency, Dr. Ibrahim Kabir, had said that his agency had certified 12 sanitation firms to assist in cleaning refuse heaps in the metropolis.
Kabir added, “We should be able to clean our environment for four hours in a month. The environment needs us too.’’
Efforts to get the current update of the cholera situation and what the government was doing to curb the spread of the disease in the state from the Executive Chairman, Primary Health Care Development Agency, Dr. Rilwan Mohammed, proved abortive as he declined comments on the matter.
Gombe doctors tackle cholera
In Gombe, it was gathered that in 2017 over 600 cases of cholera were treated and in 2021 within the first and second quarter, 178 cases had been treated and discharged with two children reportedly dead.
The affected council areas included Yalmatu Deba (Liji) and Akko (Kalajanga), with cases in Kwami and Dukku Local Government Areas.
In some villages, animals drink from the water which humans use for household purposes.
The state epidemiologist, Dr. Nuhu Bile, noted that cholera had been a recurring decimal in the state.
He said, “Usually at the beginning of the rainy season, it can be faecal-orally transmitted based on diseases people contract from eating or drinking contaminated foods. It is usually passed in faeces. The bacteria can get into the stream of water that people drink or uncooked vegetables. It goes into the intestine to present with the symptoms of diarrhoea, vomiting and dehydration if there is no intervention.
“In Kwami, an eight-year-old was brought in from Kurujul village. When they were trying to resuscitate him, we lost the child. If we got the report earlier he might have been treated. In Kalajanga, the first case was a child who started having diarrhoea and vomiting. When we got to the village, we learnt that it began at night and by morning, he died.’’
Also speaking, Dr. Kefas Zawaya of the Federal Teaching Hospital, Gombe, said that hygiene was essential in tackling cholera.
Zawaya, who is a gastroenterologist and the immediate past chairman of the state NMA, said, “Prompt reporting is key. About three years ago when I treated a young man, he exhibited diarrhoea. In the referral centre usually, when patients come, the history may present diarrhoea. So, if it has been reported maybe there is cholera in a place, but if it has not been reported the location of the person may not mean much to one until one finds out the type of stool the person is passing.’’
When one of our correspondents visited Tuduwada Primary Healthcare Centre which has turned into a referral point due to proximity and space, the facility manager, Aishatu Usman, talked about how patients were usually treated.
Usman said, “Over time after treating a patient, the relatives usually come presenting the same issue of vomiting and diarrhoea. I try as often as possible to ensure my patient is on fluid frequently to make way for recuperation if not the patient will be dehydrated.
L
“I usually interrogate patients on their source of water. There was a case in Dukku where we discovered their source of water but animals also drank from the same water so we advised them to boil water since not all of them can afford to buy packaged water. So we felt they could use the water in a way that will be most healthy by boiling it and once it is cold, they can simply filter it. This will help in minimising the cases of cholera.
Cholera management
Bile stated that containing cholera had been the responsibility of the Ministry of Health through the Public Health Emergency Operation Centre.
He said, “It is always a holistic approach and that is what we do during the beginning of every cholera season when the rains start. We always try to talk to the public through the media to remind people that it is another season for cholera so people should be watchful of what they eat. Food hygiene is paramount in the management of cholera and good disposal of sewage.’’
Zawaya said that fluid was required in managing a cholera patient.
The head of the delivery section at Gombe PHC maternity, also known as ‘Gida magani,’ Jamila Khamis, said the facility had stopped treating cholera patients, adding that management was afraid of infecting nursing mothers.
Khamis said, “We now refer to Tuduwada PHC because we don’t want nursing mothers to be infected. We don’t have the adequate site to manage them because we can infect the mothers and the newborns.’’
Also, a public health specialist, Tijani Umar, said that there were times that patients reacted to cholera treatment.
He said, “Concerning their management, there are times they react to drugs, they resist antibiotics and we change the drug.”
Challenges treating patients
The state epidemiologist said that one could never have 100 per cent compliance or a stage without cholera case hence the immediate response was vital.
Bile stated, “At the state Ministry of Health under the leadership of Dr. Habu Dahiru, the emphasis is always on quick, rapid and efficient response. At the PHEOC, what we have is a rapid response team and what we usually do daily there is that there are those who wait for signals to come from the public or any person who would call to say what is happening in their area. However, we usually get this report also, through the surveillance system in the state where we have surveillance focal persons in all the healthcare facilities who are trained to look out for diseases that can become an outbreak of which cholera is one of them. We have them in all the healthcare facilities strategically placed in Primary Healthcare Centres, cottage, specialist, general and teaching hospitals.’’
Zawaya added that adequate people had to pay for services when they come to the hospital even though there was a provision through which people could access the services and pay later.
Usman said, “There were times when two of our workers got infected. It was not so serious because immediately they got the symptoms; they took action towards getting disinfected and taking drugs.”
Treating patients, tackling disease
Bile noted that immediately there was an occurrence of the disease, the rapid response team swung into action.
He said, “We usually go out as a team; comprising a team lead, usually a doctor or an experienced healthcare worker, laboratory scientist equipped with rapid diagnostic kits.
“To treat, you need the fluid that the person is losing, and you need a shot of antibiotics and commodities for decontamination, commodities for infection control, we test, confirm and establish a rehydration point or a treatment centre. The idea is for people to receive treatment close because treating them far will further aggravate the situation. Patients can be brought in severely, moderately or mildly dehydrated.’’
On her part, Usman said that when a patient presented with cholera, he would first be given a particular drug followed by an injection to replace water and electrolyte loss in patients with low blood volume or low blood pressure.
Usman stated, “It is also used as an alkalinising agent which increases the pH level of the body. After that, we then admitted him. Note that the patient will be transfused with fluid which will serve as the food and after the patient has recovered, we then administer doxycycline to go home with and it will serve as a follow-up treatment together with zinc tablets.”
Bile noted further that once a community had been declared to have cases of cholera, they visited the community leader to assemble villagers and address them.
“We started by telling them our suspicion, reminding them of their water source after collecting samples for testing.
“Also, we try to provide alternative sources of drinking water after the health commissioner has activated the Incident Management System of cholera. It is a multiple approach that has water cooperation, they provide them with water free of charge and we also decontaminate their source of water.”
Zawaya added that personal hygiene was vital, advising that people should cultivate the habit of washing vegetables and fruit and other edibles thoroughly.
Usman however urged both medical workers and the people to obey hygiene.
Also, Khamis urged the government to build toilet facilities to reduce the spread of cholera cases. Khamis added, “As you know, open defecation is a major challenge. There should be steady disposal of refuse, so vehicles should be provided for that purpose from the point of collection from homes.”
Also, Umar called on the people to preserve their food well, from production to consumption and to treat their water.
Recently, about 61 persons were said to have recovered from cholera disease cases bringing an end to the epidemic in Kalajanga community, Akko Local Government Area of the state.
Dahiru, who declared the cholera status of the Local Government, said the disease in Kalajanga community of Akko LGA was over with the treatment and recovery of 61 persons.
“This brings an end to cholera disease in Gombe State. This declaration of an end to the infection is in line with guidelines by the World Health Organisation and NCDC. No new case has been reported over 10 days, thereby signifying an end to the outbreak. The general public is also encouraged to present themselves to health facilities if they notice symptoms like vomiting and diarrhoea,” he said.
Dahiru further said that the surveillance team of the State Ministry of Health would continue to be at alert and heighten situational awareness to carry out measures for containment and prevention of future outbreaks.
“The Ministry of Health will continue to respond to public health emergencies in line with the prioritised health agenda of Governor Muhammadu Yahaya whose timely intervention contributed to the speedy control of the disease.
“Measures taken by the ministry to mitigate the spread of the disease include activation of Incident Management System at the PHEOC, setting up of a treatment and rehydration centre at Bogo Model PHC where patients are managed free of charge.
“Others are; daily provision of potable water to affected communities by tankers of Gombe State Water Cooperation free of charge and environmental decontamination.’’
Support InfoStride News' Credible Journalism: Only credible journalism can guarantee a fair, accountable and transparent society, including democracy and government. It involves a lot of efforts and money. We need your support. Click here to Donate
